Urinary retention is the inability to empty the bladder. With chronic urinary retention, you may be able to urinate, but you have trouble starting a stream or emptying your bladder completely. You may urinate frequently; you may feel an urgent need to urinate but have little success when you get to the toilet; or you may feel you still have to go after you’ve finished urinating. With acute urinary retention, you can’t urinate at all, even though you have a full bladder. Acute urinary retention is a medical emergency requiring prompt action. Chronic urinary retention may not seem life threatening, but it can lead to serious problems and should also receive attention from a health professional.
Anyone can experience urinary retention, but it is most common in men in their fifties and sixties because of prostate enlargement. A woman may experience urinary retention if her bladder sags or moves out of the normal position, a condition called cystocele. The bladder can also sag or be pulled out of position by a sagging of the lower part of the colon, a condition called rectocele. Some people have urinary retention from rectoceles. People of all ages and both sexes can have nerve disease or nerve damage that interferes with bladder function.
What is the urinary tract?
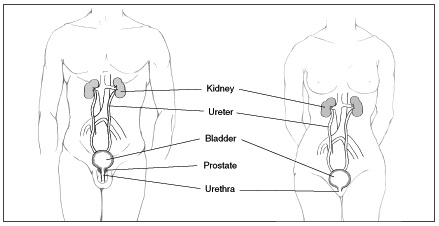
The urinary tract consists of the organs, tubes, and muscles that work together to make, move, store, and release urine. The upper urinary tract includes the kidneys, which filter wastes and extra fluid from the blood, and the ureters, which carry urine from the kidneys to the bladder. The lower urinary tract includes the bladder, a balloon-shaped muscle that stores urine, and the urethra, a tube that carries urine from the bladder to the outside of the body during urination. If the urinary system is healthy, the bladder can hold up to 16 ounces-2 cups-of urine comfortably for 2 to 5 hours.
Muscles called sphincters squeeze shut the tubes from the bladder to help keep urine from leaking. The sphincter muscles close tightly like a rubber band around the opening of the bladder, which leads into the urethra.
Nerves in the bladder tell you when it is time to urinate. As the bladder first fills with urine, you may notice a feeling that you need to go. The sensation to urinate becomes stronger as the bladder continues to fill. As it reaches its limit, nerves from the bladder send a message to the brain that the bladder is full and the urge to empty your bladder intensifies.
When you urinate, the brain signals the bladder muscle to tighten, squeezing urine out of the bladder. At the same time, the brain signals the sphincter muscles to relax. As these muscles relax, urine exits the bladder through the urethra. When all the signals occur in the correct order, normal urination occurs.
What causes urinary retention?
Urinary retention can be caused by an obstruction in the urinary tract or by nerve problems that interfere with signals between the brain and the bladder. If the nerves aren’t working properly, the brain may not get the message that the bladder is full. Even if you know that your bladder is full, the bladder muscle that squeezes urine out may not get the signal that it is time to push, or the sphincter muscles may not get the signal that it is time to relax. A weak bladder muscle can also cause retention.
Nerve Disease or Spinal Cord Injury
Many events or conditions can damage nerves and nerve pathways. Some of the most common causes are
- vaginal childbirth
- infections of the brain or spinal cord
- Diabetes
- Stroke
- accidents that injure the brain or spinal cord
- multiple sclerosis
- heavy metal poisoning
- pelvic injury or trauma
In addition, some children are born with nerve problems that can keep the bladder from releasing urine.
Infection
Infections cause swelling and irritation, or inflammation. A urinary tract infection (UTI) may cause retention if the urethra becomes inflamed and swells shut.
Surgery
During surgery, anesthesia is often administered to block pain signals, and fluid is given intravenously to compensate for possible blood loss. The combination may result in a full bladder with impaired nerve function. Consequently, many patients have urinary retention after surgery.
Medication
Many medicines work by calming overactive nerve signals. Various classes of drugs that block various signals may be used to treat allergies, stomach cramps, muscle spasms, anxiety, or depression. Some medicines are used to treat urinary incontinence and overactive bladder. The drugs that may cause urinary retention include
- Antihistamines to treat allergies
- fexofenadine (Allegra)
- diphenhydramine (Benadryl)
- chlorpheniramine (Chlor-Trimeton)
- cetirizine (Zyrtec)
- Anticholinergics/antispasmodics to treat stomach cramps, muscle spasms, and urinary incontinence
- hyoscyamine (Levbid, Cystospaz, Anaspaz, Gastrosed)
- oxybutynin (Ditropan, Ditropan XL, Oxytrol)
- tolterodine (Detrol, Detrol LA)
- propantheline (Pro-Banthine)
- Tricyclic antidepressants to treat anxiety and depression
- imipramine (Tofranil)
- amitriptyline (Elavil, Endep)
- nortriptyline (Aventyl, Pamelor)
- doxepin (Novo-Doxepin, Sinequan)
Bladder Stone
A stone formed anywhere in the urinary tract may become lodged in the bladder. If the stone is large enough, it can block the opening to the urethra like a bathtub plug.
Cystocele and Rectocele
A cystocele occurs when the wall between a woman’s bladder and her vagina weakens and allows the bladder to droop into the vagina. The abnormal position of the bladder may cause urine to remain trapped. In a rectocele, the rectum droops into the back wall of the vagina. Cystocele and rectocele are often the results of a dropping of the pelvic support floor for the bladder. This sagging can pull the bladder out of position and cause urinary problems such as incontinence or urinary retention.
Constipation
A hard stool in the rectum may push against the bladder and urethra, causing the urethra to be pinched shut, especially if a rectocele is present.
Urethral Stricture
A stricture is a narrowing or closure of a tube. Men may have a narrowing of the urethra, usually caused by scarring after a trauma to the penis. Infection is a less common cause of scarring and closure in the urethra.
What are the symptoms of urinary retention?
Acute urinary retention causes great discomfort, and even pain. You feel an urgent need to urinate but you simply can’t. The lower belly is bloated.
Chronic urinary retention, by comparison, causes mild but constant discomfort. You have difficulty starting a stream of urine. Once started, the flow is weak. You may need to go frequently, and once you finish, you still feel the need to urinate. You may dribble between trips to the toilet because your bladder is constantly full, a condition called overflow incontinence.
How is urinary retention diagnosed?
Your doctor will order a number of tests to diagnose your condition.
History of Complaints and Physical Examination
A physician will suspect urinary retention by your symptoms and will attempt to confirm the diagnosis with a physical examination of the lower abdomen. The physician may be able to feel the distended bladder by lightly tapping on your lower belly. Tapping or striking for diagnostic purposes is called percussing.
Urine Sample
A urine sample will be examined for signs of infection, which may be a cause or a result of urinary retention.
Bladder Scan
A bladder scan uses a portable ultrasound device that can determine how much urine is in your bladder. You will be asked to urinate, and then your doctor or nurse will use the bladder scan to determine the post-void residual (PVR). The word residual refers to the amount of urine left in the bladder after urination. If you typically have a PVR of 100 milliliters or more, you are considered to have chronic urinary retention.
Cystoscopy
Your doctor may use a cystoscope to see inside your bladder and urethra. The cystoscope has lenses like a telescope or microscope. These lenses let the doctor focus on the inner surfaces of the urinary tract.
Some cystoscopes use optical fibers made of flexible glass that carry an image from the tip of the instrument to a viewing piece at the other end. The fiber-optic cystoscope is as thin as a pencil and has a light at the tip. The doctor can use the cystoscope to find and perhaps remove a stone that may be blocking the bladder opening. The device can help the doctor identify narrowing of the urethra from prostate enlargement or UTI.
X Ray and Computerized Tomography (CT) Scan
A conventional x ray may show a spot where the urinary tract is narrowed or obstructed. It may show that the bladder is out of its normal position. CT scans use multiple x-ray images to construct a better view of internal organs, which may help find stones or other obstructions.
Urodynamic Tests
Urodynamic tests include different techniques to measure the bladder’s ability to empty steadily and completely. In a pressure flow study, you will be asked to empty your bladder so that a special catheter can measure the pressure required to start a stream. This pressure flow study helps to identify bladder outlet obstruction from prostate enlargement or cystocele.
If your doctor or nurse thinks your urinary problem is related to nerve damage, you may be given an electromyography. This test measures the muscle activity in the urethral sphincter using sensors placed on the skin near the urethra and rectum. Sometimes the sensors are on the urethral or rectal catheter. A catheter is a thin, flexible tube that can be guided essay help into openings of the body. Muscle activity is recorded on a machine. The patterns of the impulses will show whether the messages sent to the bladder and urethra are coordinated correctly.
How is urinary retention treated?
Catheterization
With acute urinary retention, treatment begins with the insertion of a catheter through the urethra to drain the bladder. This initial treatment relieves the immediate distress of a full bladder and prevents permanent bladder damage. Long-term treatment for any case of urinary retention depends on the cause.
The cause of acute urinary retention may be temporary. For example, if you have retention after surgery, you will probably regain your ability to urinate after the effects of the anesthesia wear off. In such cases, you may need to have a catheter inserted once or twice with no other treatment required after you have shown you can urinate on your own.
If you have chronic urinary retention, or if acute retention appears to become chronic, further treatment will be necessary. You may need to continue using a catheter if other options do not work for you. You may be taught to catheterize yourself as needed. You will need to learn sterile technique to avoid UTIs.
Surgery for Women with Cystocele or Rectocele
Women may need surgery to lift a fallen bladder or rectum. The most common procedure for cystocele and rectocele repair is for the surgeon to make an incision in the wall of the vagina to find the defect or hole in the membrane-a wall of tissue called fascia-that normally separates the vagina from the other pelvic organs. The surgeon places sutures in the fascia to close up the defect, then closes the incision in the vaginal wall with more stitches, removing any excess tissue. These suturing steps tighten the layers of tissue that separate the organs, creating more support for the pelvic organs.
What are the complications of urinary retention?
Urinary Tract Infection
Urine is normally sterile, and the normal flow of urine usually prevents bacteria from growing in the urinary tract. When urine stays in the bladder, however, bacteria have a chance to grow and infect the urinary tract.
Bladder Damage
If the bladder becomes stretched too far or for long periods, the muscle may be permanently damaged and lose its ability to contract.
Chronic Kidney Disease
If urine backs up into the kidneys, permanent kidney damage can lead to reduced kidney function and chronic kidney disease. If you lose too much of your kidney function, you will need dialysis or a kidney transplant to stay alive.
What are the complications of treatments for urinary retention?
UTI from Catheter Use
Placement of a urinary catheter provides an opportunity for bacteria to enter the urinary tract. Bacteria may come from the patient’s anus and perineum or from the health worker’s hands. Health workers must take great care, using sterile technique, when placing a catheter. If you are performing clean intermittent catheterization, you must follow the same sterile procedures every time you handle the catheter.


